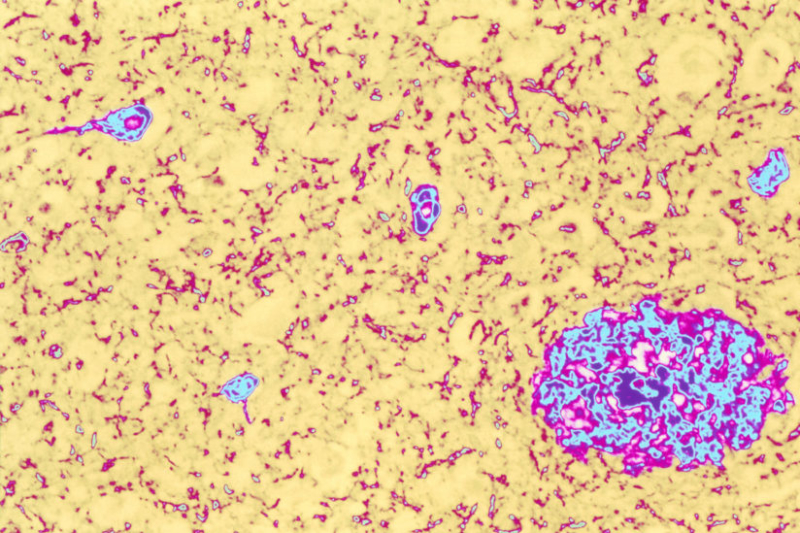
 Colored light micrograph of brain tissue from an Alzheimer's disease sufferer. Both of the classic pathological features of this disease are seen here. Both of these abnormalities disrupt the normal working of the brain. The symptoms of Alzheimer's Disease include memory loss (particularly of recent events), disorientation and mood changes. Death occurs after several years of decline, and there is no cure. Magnification: x50 at 6x7cm size.
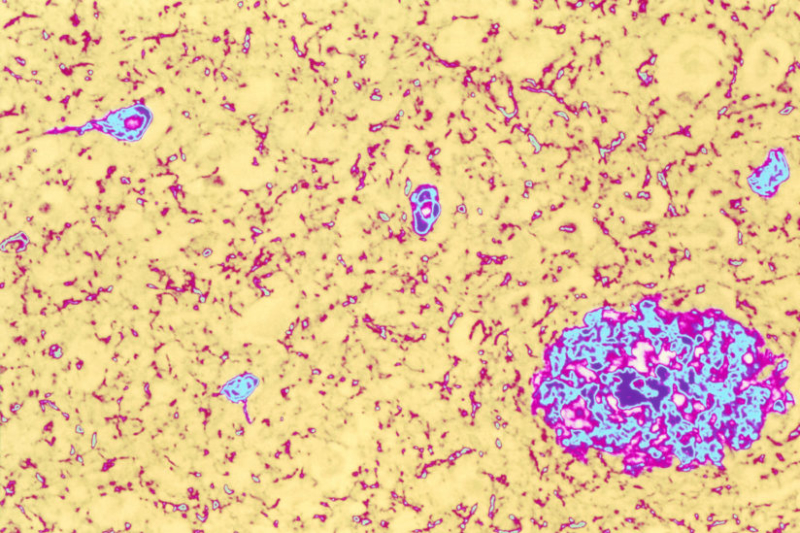
Colored light micrograph of brain tissue from an Alzheimer's disease sufferer. Both of the classic pathological features of this disease are seen here. Both of these abnormalities disrupt the normal working of the brain. The symptoms of Alzheimer's Disease include memory loss (particularly of recent events), disorientation and mood changes. Death occurs after several years of decline, and there is no cure. Magnification: x50 at 6x7cm size.
(Image/Simon Fraser, Science Source)
Keck School of Medicine of USC is launching a large clinical study to determine whether a man-made antibody would slow or stop the progression of Alzheimer’s disease by targeting memory-robbing plaques in the earliest stages of the illness.
Described as a public-private partnership, the AHEAD 3-45 Study will be conducted with funding from the National Institute on Aging, part of the U.S. National Institutes of Health (NIH), and Japanese pharmaceutical company Eisai Inc., the U.S. pharmaceutical subsidiary of Eisai Co., Ltd. The trial will be run by and as part of the NIH-funded Alzheimer’s Clinical Trial Consortium (ACTC).
The study will be led by Paul Aisen, director of USC’s Alzheimer’s Therapeutic Research Institute (ATRI) in San Diego, and Reisa Sperling and Keith Johnson from Brigham and Women’s Hospital and Massachusetts General Hospital, Harvard Medical School, in partnership with Eisai. ATRI is part of the Keck School of Medicine.
USC emphasizes “a strong commitment to sharing data”
“Alzheimer’s disease is an urgent problem, with almost 6 million Americans plus their loved ones affected by this illness,” said Laura Mosqueda, dean of the Keck School of Medicine and professor of geriatrics and family medicine. “ATRI’s expertise in clinical trial design and implementation and data analysis, along with a strong commitment to sharing data to advance the field, makes me confident USC will make significant progress in identifying a treatment for this terrible disease.”
USC is one of the leading private research institutions studying the disease. NIH funding for Alzheimer’s research at USC more than quintupled to $68 million in 2018 from $13.3 million in 2015.
There is no cure for Alzheimer’s, and the problem is growing as more Americans are diagnosed with the disease. USC researchers project that, by 2050, the number of Americans diagnosed with Alzheimer’s will have risen to nearly 14 million and health care costs will have tripled to $1.1 trillion annually.
Aisen is among 100 USC researchers who study the memory-robbing illness, searching for potential therapies and analyzing its impact on the health care system and its toll on caregivers. Along with Sperling and Ronald C. Petersen, director of the Mayo Clinic Alzheimer’s Disease Research Center and professor of neurology at Mayo Clinic College of Medicine and Science, Aisen is co-director of ACTC.
Alzheimer’s drug designed to bind to amyloid
The drug in the upcoming study — BAN2401, delivered intravenously — is designed to bind to a sticky, toxic protein called beta amyloid. The binding neutralizes beta amyloid and helps “tag” it, so the immune system can recognize it and clear it from the brain. Many scientists believe that amyloid accumulation in the brain is the inciting event in Alzheimer’s disease.
“We know that BAN2401 treatment is effective at reducing amyloid deposits in the brain, as shown by the normalization of amyloid PET scans,” Aisen said. “Our study will determine the impact of amyloid removal on cognitive decline and biological markers of Alzheimer’s disease when administered to people who do not yet have substantial, irreversible damage from Alzheimer’s.”
BAN2401 is a humanized monoclonal antibody comprised of aggregated forms of Aβ, including protofibrils, as an antigen. It is based on the research of cases of Swedish familial Alzheimer’s disease with Arctic mutation, which concluded abnormal accumulation of Aβ protofibrils may be a cause of Alzheimer’s disease onset.
A previous phase 2 study showed that BAN2401 removes brain amyloid and possibly slows cognitive decline. Investigators hope that administration of BAN2401 very early in the disease, before symptoms occur, may significantly slow disease progression. While BAN2401 is being studied in other clinical trials, the USC study will incorporate the exploration of biomarkers using positron emission tomography (PET) scans and cerebrospinal fluid measures.
9,000 individuals to be recruited globally to study Alzheimer’s drug
For this four-year study, about 9,000 individuals recruited from 100 sites globally will be screened to find 1,400 people who are clinically normal and have intermediate or elevated levels of amyloid in their brains. Researchers hope to screen the first participant by May 31 and complete enrollment in 18 to 30 months.
The study group will be divided into two double-blind sub-studies named “A3” and “A45.” Study participants will be randomly assigned to receive the drug or the placebo. Neither the participants nor the scientists will know who is receiving a particular treatment.
The A3 sub-study will include 400 cognitively normal participants with intermediate levels of amyloid as determined by amyloid PET scan, who are at high risk for further amyloid buildup. They will get intravenous infusions of BAN2401, or a placebo, every four weeks for 216 weeks.
The A45 sub-study will include 1,000 participants with little to no cognitive impairment who have elevated levels of amyloid in the brain and are at high risk for progression to mild cognitive impairment and Alzheimer’s dementia. The study will test whether high-dose BAN2401 every two weeks for 96 weeks can clear amyloid buildup and, afterward, whether further doses of BAN2401 could prevent plaque from reappearing.
“Amyloid deserves the attention we have given it,” Aisen said. “Amyloid accumulation begins the disease process, and it predicts progressive cognitive decline to dementia. All of the known genetic causes of Alzheimer’s disease are tightly linked to amyloid accumulation.”
— by Leigh Hopper
The A3 sub-study is funded by NIH grant R01AG054029 and is affiliated with ACTC. The A45 sub-study is funded through the ACTC, NIH grant R01AG061848. ACTC is funded by NIH grant U24AG057437.